
For individuals struggling with alcohol addiction, seeking professional help is crucial for both their overall well-being and circulatory system health. Alcohol abuse can have severe consequences on the cardiovascular system and increase the risk of various health conditions. Increased autophagy as a possible mechanism underlying the adverse myocardial effects of ethanol is intriguing. This is especially true in light of the relationship between a sensor of stress (mTOR) and nutrient deprivation and how essential autophagy is to cell survival. As noted above, chronic alcohol exposure leads to a decrease in mTOR activity, which corresponds to increased markers of autophagy (Lang and Korzick 2014). The autophagy pathway also is rapidly upregulated during ATP depletion, mitochondrial dysfunction, and oxidative stress.
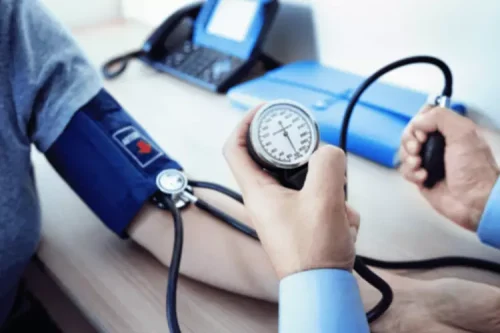
Alcohol’s Effects on Blood Pressure and Incident Hypertension
You probably already know that excessive drinking can affect you in more ways than one. Of course, healthcare professionals are here to assist and support you along the way. There’s more than one kind of blood thinner, and they work in different pathways within the body.
What are the risks of drinking alcohol when on my medication?
- Beyond the effects on bleeding and healing, excessive alcohol consumption can contribute to a range of other health risks.
- “It’s important to understand drug-food interactions when you’re taking a blood thinner like warfarin (Coumadin®) the most common one,” warns Dr. Bishop.
- Additionally, it is vital to regularly attend follow-up appointments with a healthcare professional to monitor the effectiveness of treatment and discuss any concerns or side effects.
- Always discuss any supplements you’re taking or considering with your healthcare provider, as they can interfere with other medications.
- Alcohol affects how well your blood clots, potentially negating the effects of the blood thinners or increasing them to a dangerous level.
- They’ll also help you learn how to minimize the risks of taking a blood thinner so you can reap the rewards without worry.
The same is true if brushing or flossing your teeth start to cause bleeding. Other signs of thin blood include nosebleeds and abnormally heavy menstrual flow. Green tea also contains some vitamin K, so it’s best to choose another option, like black tea, which doesn’t interact with a blood thinner. If you’re taking warfarin, you don’t have to give up foods higher in vitamin K completely. But limiting them in your diet and being consistent in the portions you do eat is important. Changing up how much vitamin K you’re getting each day can prevent warfarin from doing its job.
Interactions with Medications and Health Conditions
- These data highlight how gender may be an important modifier of the alcohol threshold level and can shape the alcohol benefit–risk relationship.
- Bleeding during surgery can increase the length of time a person needs to stay in the hospital and increase the risk of complications and death.
- Understanding these aspects is crucial for individuals who want to make informed choices regarding their alcohol intake.
- If you take a drug to restore your platelet levels, it could be a few months or a year before your levels are healthy again.
- Both the negative and positive effects of alcohol use on particular CV conditions are presented here.
- Different levels of daily wine consumption (i.e., sometimes, 1 to 2 glasses/day, and ≥3 glasses/day) had no effect on fatal or nonfatal outcomes (e.g., hospitalization for a CV event).
Healthcare professionals treat AUD with medications and behavioral therapies. They may also recommend joining a support group for individuals with AUD. This article discusses the effects that alcohol has on the blood in both the short and long term. Keep reading to learn more about this blood-thinning effect, how alcohol interacts with blood-thinning medications, and more. A person with substance use disorder should not attempt to stop using alcohol abruptly before surgery, as this could lead to alcohol withdrawal syndrome.

There are too many variables to make a blanket statement that alcohol is good for your blood pressure. Light drinking (one or two drinks) can lower your blood pressure, but that doesn’t mean it’s good for you. Many of the studies that make blood thinners and alcohol this claim do not consider other lifestyle choices, like diet and exercise, which have a much bigger impact on blood pressure. However, that does not mean that drinking is healthy, nor should you use alcohol to manage your blood pressure.
Side Effects of Blood Thinners
Despite the progress in standardizing measurement of alcohol, studies still vary in how they define the different levels of drinking, such as low-risk or moderate and heavy drinking. Most often, low-risk or moderate drinking has been defined as 1 to 2 standard drinks per day and heavy alcohol consumption as 4 or more standard drinks per day. However, ascertaining the exact alcohol consumption threshold for determining both the benefit and risk has been challenging, and threshold levels continue to differ across studies. You should limit your alcohol intake if you are taking blood thinners.
It’s essential to approach alcohol consumption responsibly and be mindful of its potential impact on our overall health and well-being. This article explores how alcohol affects the ability of the blood to clot. Finally, it answers some common questions about alcohol and blood thinning. But sometimes, a blood clot can form in — or travel to — an artery that supplies your heart or brain with oxygen-rich blood. This may lower your risk for the type of strokes caused by blockages in blood vessels.
Moderate Alcohol Use and Reduced Heart Disease Risk

The program offers structured therapies, constant medical supervision, and a supportive community to promote independence, improve function, and enhance overall well-being. The proportion of cardiomyopathy cases attributable to alcohol abuse has ranged from 23 to 40 percent (Piano and Phillips 2014). Recently, Guzzo-Merello and colleagues (2015) reported that, among 282 patients with a dilated cardiomyopathy phenotype, 33 percent had ACM. Alcohol may affect various mechanisms implicated in ischemic preconditioning.
Different anticoagulants work at different parts of the coagulation process. For instance, some anticoagulants do this by competing with vitamin K, which your body needs to make proteins called clotting factors. When it comes to alcohol consumption and its impact on blood thinning, there are both potential benefits and risks involved.
- Make sure to tell your doctor about all the medications you’re taking.
- The process of blood clotting is very complex, with multiple chains of chemical reactions called the “clotting cascade” that must occur to develop a blood clot.
- Your doctor may tell you to limit your participation in contact sports to reduce the chance of bleeding.
- Alcohol should be avoided when taking Coumadin, as it is one of the most serious risk factors for complications with this medication.
However, higher amounts of alcohol consumption may have the opposite effect and increase the risk of blood clotting. Research suggests drinking alcohol may thin the blood by affecting platelets, which are the parts of blood that initiate coagulation, or clotting. The amount of alcohol a person consumes daily contributes to how it affects blood and heart health. New research has found that moderate consumption, meaning one or two drinks per day, can decrease cardiovascular disease risk. While the mechanism behind why this happens is unclear, the theory is that this moderate consumption reduces stress reactivity in the brain.
